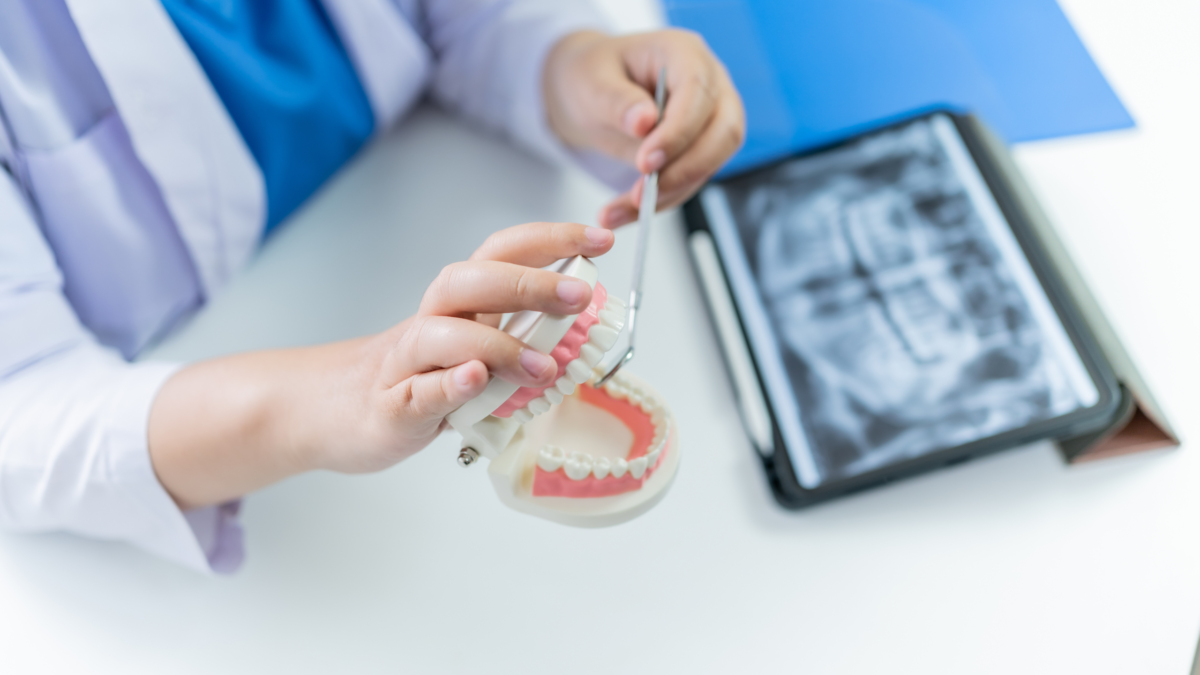
Maximizing Revenue and Efficiency: The Benefits of Behavioral Health Billing with Optimal Billing Solutions
April 5, 2024
The Role of Optimal Billing Solutions in Maximizing Medical Grant Benefits for Higher Education Institutions
May 3, 2024Myofascial and oral surgery are two closely related medical specialties that deal with the treatment of conditions affecting the muscles, soft tissues, and bones in the head, neck, and face. While both these fields focus on improving patients' overall health and well-being, they also involve complex billing practices that can be challenging to navigate.
In this blog, we will provide an overview of myofascial and oral surgery medical billing to help you understand the complexities involved in this process.
What is Myofascial Medical Billing?
Myofascial medical billing refers to the process of submitting claims for services provided by healthcare professionals specializing in treating myofascial pain syndrome (MPS). This condition affects the connective tissue or fascia surrounding muscles, causing chronic pain, muscle stiffness, and limited movement.
To accurately bill for myofascial services, healthcare providers must have a thorough understanding of Current Procedural Terminology (CPT) codes specific to MPS treatments. These codes describe the procedures performed during a patient's visit, such as trigger point injections or manual therapy techniques.
Additionally, most insurance companies require supporting documentation from providers to validate the necessity of these treatments. This includes detailed notes about a patient's symptoms and progress throughout their treatment plan.
What is Oral Surgery Medical Billing?
Oral surgery medical billing involves submitting claims for services provided by dental surgeons who specialize in diagnosing and treating conditions affecting the mouth, jawbones, teeth, and facial structures. These may include procedures such as tooth extractions, dental implants placement or repair surgeries for cleft lip/palate abnormalities.
Similar to myofascial medical billing, accurate coding is crucial in oral surgery billing. Dental surgeons must use CDT (Current Dental Terminology) codes when filing claims for procedures performed during a patient's visit.
Understanding the Basics: What is Myofascial and Oral Surgery?
Myofascial and oral surgery are two types of medical procedures that are often confused with each other due to their similar names. However, they are distinct in terms of the conditions they treat and the billing practices involved. In this section, we will delve into the basics of myofascial and oral surgery to help you better understand these procedures.
Myofascial surgery is a type of procedure that focuses on treating pain or dysfunction in the soft tissues, specifically the myofascial structures in our body. These structures include muscles, tendons, ligaments, and fascia - a connective tissue that surrounds and supports these structures. Myofascial pain can be caused by various factors such as trauma, repetitive strain injuries, or chronic conditions like fibromyalgia. The goal of myofascial surgery is to release tension in these soft tissues to alleviate pain and improve function.
On the other hand, oral surgery involves surgical procedures performed on the mouth, jaws, face, and neck region. It includes a wide range of treatments such as wisdom tooth extraction, dental implants placement, corrective jaw surgeries, and treatment for facial trauma or deformities. Oral surgeons are highly trained specialists who have completed both dental and medical degrees to perform these complex procedures.
Both myofascial and oral surgeries require specialized training and expertise from healthcare professionals. However, there are significant differences when it comes to their billing practices.
In general terms, insurance companies typically cover oral surgeries under medical plans while myofascial surgeries fall under physical therapy or chiropractic care benefits. This means that patients undergoing an oral surgery would need pre-authorization from their medical insurance provider while those undergoing a myofascial procedure would require approval from their physical therapy/chiropractic insurance provider.
Another key difference in billing between these two types of surgeries is related to coding systems used by healthcare providers for reimbursement purposes. Oral surgeons use Current Procedural Terminology (CPT) codes, which are specific to medical procedures, while myofascial surgeries use physical therapy or chiropractic-specific codes.
Understanding the basics of myofascial and oral surgery is crucial in comprehending their billing practices. While they may have similar names and involve specialized surgical skills, they treat different conditions and require different billing processes. It is essential to consult with your healthcare provider and insurance company for a clear understanding of coverage and reimbursement for these procedures.
Differences in Treatment and Services Offered
Myofascial and oral surgery are two distinct types of procedures that often require different treatment and services. As a result, the billing practices for these procedures can also vary significantly.
One major difference in treatment between myofascial and oral surgery is the type of condition or issue being addressed. Myofascial surgery involves treating problems with the fascia, which is the connective tissue surrounding muscles, while oral surgery focuses on issues within the mouth, jaw, and face. These differences in treatment also mean that different specialists may be involved in each procedure. For example, a myofascial surgeon may work closely with physical therapists to address muscle dysfunction, while an oral surgeon may collaborate with dentists or orthodontists for pre- or post-surgery care.
As a result of these varying treatments and specialists involved, the services offered during myofascial and oral surgeries can differ as well. Myofascial surgery typically involves more manual techniques such as soft tissue manipulation and trigger point therapy to release tension in the fascia. In contrast, oral surgeries may involve more invasive procedures such as extractions or dental implants. Additionally, anesthesia options may differ between these procedures – local anesthesia is commonly used for myofascial surgeries while general anesthesia may be necessary for certain types of oral surgeries.
Another important difference to note is that myofascial surgeries are often considered “medically necessary” while oral surgeries are often categorized as “dental procedures.” This distinction can impact insurance coverage and reimbursement rates. While most health insurance plans cover medically necessary procedures, dental insurance plans have limited coverage for dental procedures.
The variations in treatment and services offered also affect how these procedures are billed to insurance companies. Myofascial surgeries usually fall under medical billing codes such as Current Procedural Terminology (CPT) codes, while oral surgeries use dental billing codes known as Current Dental Terminology (CDT) codes. These codes are necessary for insurance companies to accurately determine coverage and reimbursement rates for each procedure.
There are several key differences in treatment and services offered between myofascial and oral surgeries. From the type of condition being addressed to the specialists involved, these distinctions have a significant impact on billing practices and insurance coverage. It is important for patients to understand these differences in order to be fully informed about their treatment options and potential costs associated with each procedure.
The Importance of Proper Medical Coding for Reimbursement
Proper medical coding is an essential aspect of the reimbursement process in healthcare. It involves assigning standardized codes to medical procedures and services, which are then used for billing purposes. Accurate coding is crucial to ensure that healthcare providers receive timely and adequate reimbursement for the services they provide.
One of the primary reasons why proper medical coding is essential for reimbursement is because it helps avoid claim denials. Insurance companies use these codes to determine whether a particular service or procedure is covered under a patient's insurance plan. If the code does not match the service provided, the claim may be denied, resulting in delayed or no payment for the provider. This can lead to financial loss and impact the quality of care that can be offered to patients.
Moreover, incorrect coding can also result in overbilling or underbilling, both of which can have severe consequences. Overbilling occurs when a code assigned to a service or procedure indicates more complex work than was actually performed, leading to higher reimbursement rates. Underbilling happens when a less complicated code is used, resulting in lower reimbursements than what was deserved by the provider. Both these scenarios can result in significant financial losses for healthcare facilities and affect their ability to continue providing quality care.
Proper medical coding also plays a crucial role in maintaining compliance with regulatory bodies such as Medicare and Medicaid. These programs have specific guidelines for coding practices, and any errors or discrepancies can result in audits and penalties for healthcare providers. By ensuring accurate coding practices, providers can avoid potential legal issues and maintain their reputation within the industry.
In addition to avoiding denials and maintaining compliance, proper medical coding also enables accurate tracking of patient care data. With standardized codes, it becomes easier to analyze trends in treatments and procedures provided by healthcare facilities. This information can help improve overall patient care by identifying areas where there may be gaps or room for improvement.
Furthermore, accurate medical coding contributes significantly to revenue cycle management (RCM). The RCM process involves all the steps taken by healthcare facilities to ensure timely and full reimbursement for the services they provide. Accurate coding is a crucial component of RCM, as it ensures that insurance claims are processed correctly and payments are received promptly.
Proper medical coding is vital for accurate and timely reimbursement in the healthcare industry. It helps avoid claim denials, maintain compliance with regulations, track patient care data, and contribute to effective revenue cycle management. Therefore, healthcare providers must prioritize ensuring accurate coding practices to receive fair compensation for their services.
Common Challenges Faced in Myofascial and Oral Surgery Billing
Myofascial and oral surgery billing can be quite complex and challenging for healthcare providers. These types of surgeries involve intricate procedures and often require multiple visits, making the billing process more complicated than other medical specialties. In this section, we will discuss some of the common challenges faced by healthcare providers when it comes to myofascial and oral surgery billing.
-
Coding Accuracy:
One of the most significant challenges in myofascial and oral surgery billing is ensuring coding accuracy. Due to the complexity of these procedures, there is a higher chance of errors in coding, resulting in claim denials or delays in reimbursement. It is crucial for healthcare providers to have a thorough understanding of the different codes associated with these surgeries and ensure they are using them correctly.
-
Understanding Insurance Coverage:
Another challenge faced by healthcare providers is navigating through insurance coverage for myofascial and oral surgeries. Different insurance companies may have varying policies on what they cover, which can lead to confusion and discrepancies in claims processing. Providers must stay updated on insurance policies to avoid any misunderstandings or denials.
-
Time-Consuming Process:
The billing process for myofascial and oral surgeries can also be time-consuming due to the extensive documentation required for these procedures. Healthcare providers must document all aspects of the treatment thoroughly, including diagnosis, treatment plans, details of surgical procedures, etc., which can be time-consuming.
-
Coordination with Multiple Providers:
In many cases, patients undergoing myofascial or oral surgery may require care from multiple specialists such as dentists, surgeons, orthodontists, etc. This coordination between different providers can present another challenge in terms of billing since each provider needs to bill separately for their services accurately.
-
Prior Authorization Requirements:
Insurance companies often require prior authorization before covering certain treatments or procedures related to myofascial and oral surgeries. Obtaining prior authorization can be a lengthy process that involves detailed paperwork and documentation, which can be challenging for healthcare providers.
-
Keeping Up with Changing Regulations:
The healthcare industry is constantly evolving, and billing regulations are no exception. Healthcare providers need to stay updated on any changes in coding guidelines, insurance policies, or other regulations that may impact the billing process for myofascial and oral surgeries.
Myofascial and oral surgery billing present various challenges that healthcare providers must navigate through to ensure timely reimbursement. It is crucial for providers to have a strong understanding of these challenges and develop effective strategies to overcome them efficiently.
Tips for Efficient and Accurate Billing Practices
Efficient and accurate billing practices are crucial for both myofascial and oral surgery procedures. Proper billing ensures that healthcare providers receive timely payments for their services, while also helping patients understand the costs associated with their treatment. In this section, we will discuss some practical tips to help streamline your billing process and ensure accuracy.
- Verify Insurance Information: The first step in efficient billing is to verify the patient's insurance information before any treatment is provided. This includes checking their coverage details, co-pays, deductibles, and any special requirements or restrictions. This will save time and prevent unexpected payment issues down the line.
- Clearly Communicate Treatment Plans: It is important to have open communication with your patients regarding their treatment plan and associated costs. Make sure they are aware of any out-of-pocket expenses they may incur and provide them with a detailed breakdown of the expected charges. This will help avoid confusion or disputes later on.
- Develop a Consistent Billing System: Having a consistent system in place for all your billing tasks can greatly improve efficiency and accuracy. This includes using standardized codes for procedures, maintaining proper documentation, and regularly updating fee schedules.
- Stay Up-to-Date with Coding Changes: Medical coding is constantly evolving, so it is essential to stay updated on any changes to ensure accurate billing. Keep track of new codes that may affect your practice and make necessary adjustments to your system accordingly.
- Modernize Your Billing Process: With advancements in technology, there are now numerous software options available that can streamline your entire billing process – from scheduling appointments to generating invoices. These tools not only save time but also reduce the chances of human error.
- Hire Competent Staff: Hiring knowledgeable staff who understand coding requirements can significantly improve the accuracy of your billing process. Conduct regular training sessions to keep them updated on changes in medical coding guidelines.
- Regularly Review Claims: It is crucial to review claims before submitting them to insurance companies for accuracy and completeness. This will help avoid delays in payments or rejections due to errors.
Efficient and accurate billing practices are essential for both myofascial and oral surgery procedures. By implementing these tips, healthcare providers can streamline their billing process, reduce errors, and ensure timely payment for their services.
Why Understanding Myofascial and Oral Surgery Billing Matters
It is clear that understanding myofascial and oral surgery billing is crucial for both healthcare providers and patients. These two types of procedures may seem similar, but they have distinct differences in terms of treatment approach, billing codes, and reimbursement rates. By having a thorough understanding of these differences, providers can ensure accurate coding and billing practices, leading to timely reimbursements and avoiding potential legal issues.
Moreover, for patients, being aware of the different billing practices can help them make informed decisions about their treatment plans. They can also better understand their insurance coverage and any out-of-pocket expenses they may incur.
One key takeaway from this discussion is the importance of proper documentation in ensuring correct billing for myofascial and oral surgeries. Providers must accurately document all aspects of the procedure to justify the use of specific codes for reimbursement purposes. This includes documenting patient history, pre-operative assessment, intra-operative details, post-operative care instructions, as well as any complications or unexpected findings during the procedure.
Another crucial aspect is staying updated with current coding guidelines and regulations set by insurance companies. As mentioned earlier, there are differences in how myofascial vs. oral surgery procedures are coded and billed by different insurers. Therefore, it is essential to regularly review these guidelines to avoid any errors that could result in claim denials or delays in reimbursement.
Furthermore, understanding the complexities of myofascial vs. oral surgery billing also highlights the need for effective communication between healthcare providers and insurance companies. Clear communication ensures that claims are submitted correctly with all necessary documentation attached to avoid any misunderstandings or disputes over payments.
Myofascial release therapy offers numerous benefits for patients suffering from muscle pain or dysfunction due to various causes such as trauma or chronic diseases like fibromyalgia. On the other hand, oral surgery procedures address more complex dental issues that require specialized treatment. As healthcare providers, understanding the distinct billing practices for these two procedures is essential in providing quality care to patients and avoiding any financial or legal implications. Patients, too, can benefit from this knowledge by being informed about their insurance coverage and treatment options. A thorough understanding of myofascial and oral surgery billing matters greatly impacts the success of these procedures for both providers and patients alike.